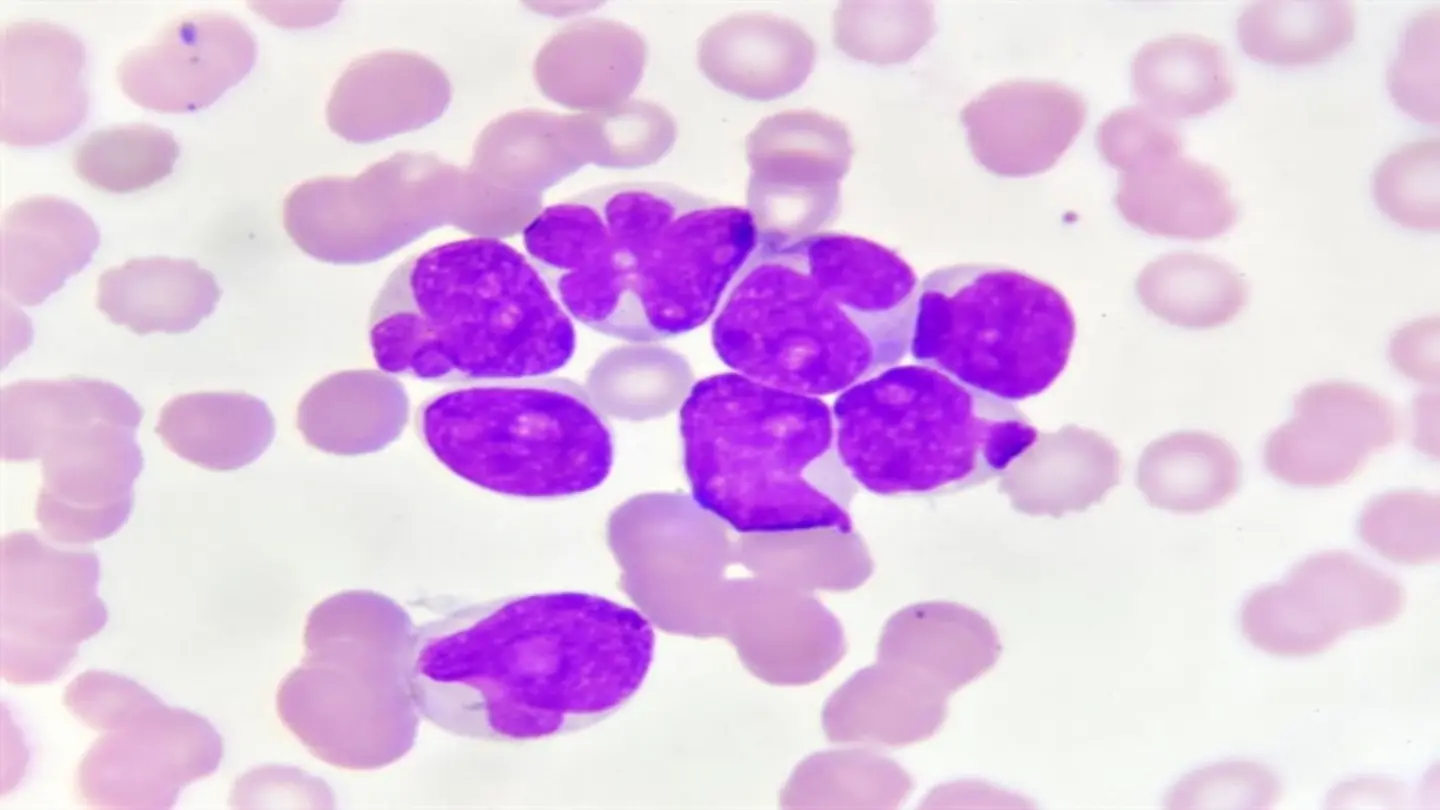
New research published in the European Medical Journal details the development of nomograms – predictive modeling tools – designed to forecast survival probabilities for patients diagnosed with acute erythroid leukemia (AEL). AEL is a rare and aggressive subtype of acute myeloid leukemia (AML), characterized by a predominant proliferation of immature red blood cells. Accurate prognosis is crucial for guiding treatment decisions and providing patients with realistic expectations.
Currently, risk stratification in AEL relies heavily on traditional cytogenetic and clinical factors. However, these methods often lack the precision needed to individualize treatment plans. The study addresses this gap by integrating a wider range of variables into the nomograms, including age, performance status, white blood cell count, hemoglobin levels, and the presence of specific genetic mutations.
Developing the Predictive Models
Researchers retrospectively analyzed data from a substantial cohort of AEL patients. They employed sophisticated statistical techniques, including Cox proportional hazards regression, to identify independent prognostic factors. These factors were then incorporated into the nomograms, allowing clinicians to estimate the probability of overall survival (OS) and progression-free survival (PFS) at various time points.
The nomograms were constructed and validated using multiple datasets to ensure their robustness and generalizability. Validation processes included assessing the nomograms’ discriminatory ability – their capacity to differentiate between patients with different survival outcomes – and calibration – the accuracy of their predicted probabilities. The results demonstrated that the nomograms exhibited superior predictive performance compared to existing risk stratification systems.
The study highlights the importance of considering a comprehensive set of clinical and genetic parameters when assessing the prognosis of AEL. Specifically, the inclusion of genetic mutations, such as those in the TP53, RUNX1, and NPM1 genes, significantly improved the accuracy of the predictions. These mutations are known to influence the behavior of leukemia cells and their response to therapy.
The researchers emphasize that these nomograms are intended to be used as a decision support tool for clinicians, rather than a replacement for clinical judgment. They acknowledge that further prospective validation is needed to confirm the nomograms’ clinical utility and refine their predictive accuracy. However, the initial findings suggest that these tools have the potential to significantly improve the management of AEL patients.
Ultimately, the goal is to personalize treatment strategies based on an individual patient’s risk profile, maximizing the chances of achieving long-term remission and improving overall survival. The development of these nomograms represents a significant step forward in achieving this goal for individuals battling this challenging form of leukemia. The research team plans to make the nomograms readily accessible to clinicians through an online platform, facilitating their widespread adoption and implementation in clinical practice.
Image Source: Google | Image Credit: Respective Owner