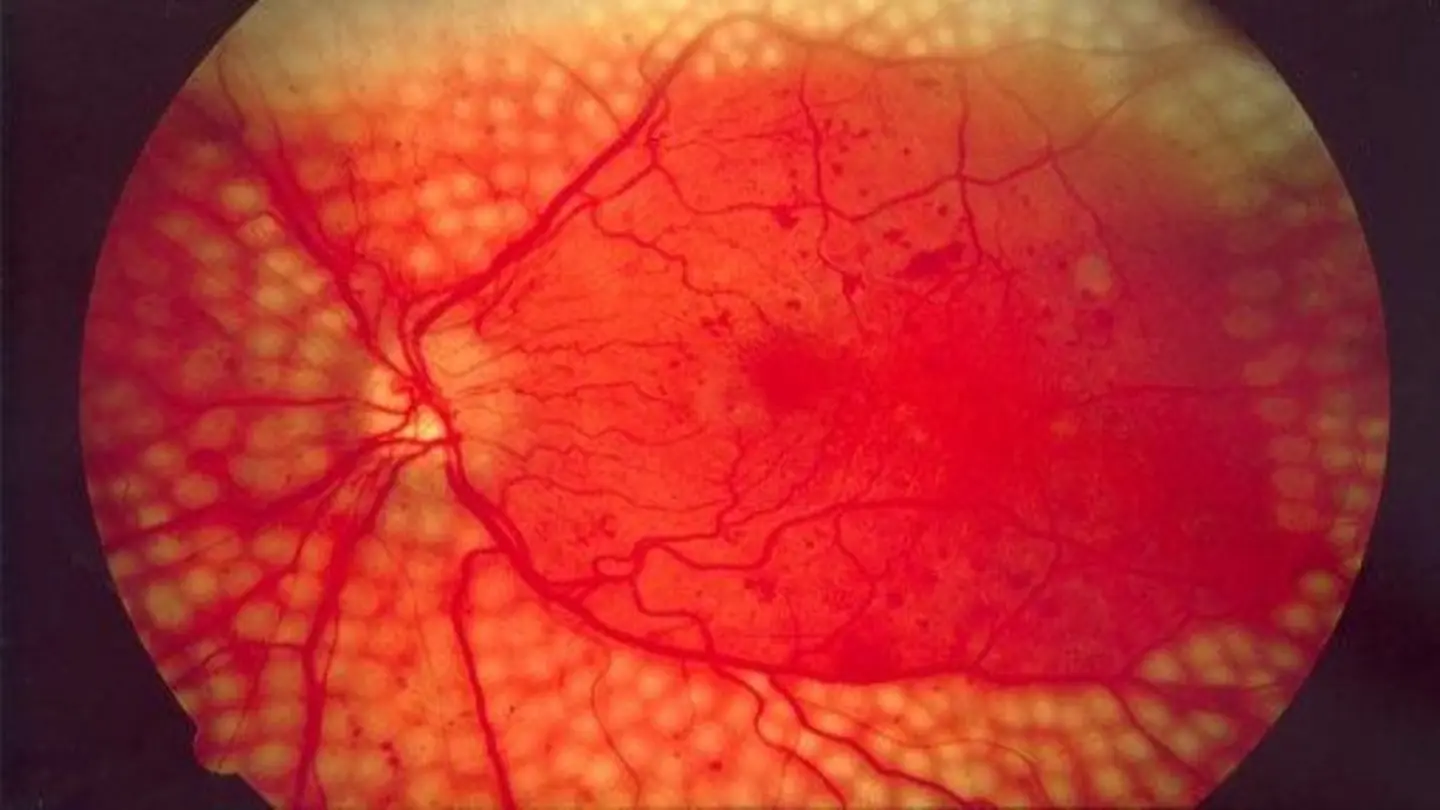
Diabetic retinopathy, a common complication of diabetes, poses a significant threat to vision, potentially leading to blindness. Early detection through regular screening is crucial for managing the condition and preventing irreversible damage. Yale Medicine experts emphasize the importance of proactive eye care for individuals with diabetes.
Diabetes affects blood vessels throughout the body, including those in the retina, the light-sensitive tissue at the back of the eye. High blood sugar levels can damage these vessels, causing them to leak fluid or bleed. In the early stages, diabetic retinopathy may not cause any noticeable symptoms. As the condition progresses, it can lead to blurred vision, floaters, dark spots, and eventually, vision loss.
Understanding the Stages of Diabetic Retinopathy
Diabetic retinopathy progresses through several stages. Initially, it may manifest as mild non-proliferative retinopathy, characterized by small areas of swelling in the retina. As the condition worsens, it can advance to moderate or severe non-proliferative retinopathy, with more pronounced blood vessel damage. The most advanced stage is proliferative retinopathy, where new, abnormal blood vessels grow on the surface of the retina. These new vessels are fragile and prone to bleeding, which can lead to scarring and retinal detachment.
Regular screening is essential for detecting diabetic retinopathy in its early stages, when treatment is most effective. The American Academy of Ophthalmology recommends that individuals with type 1 diabetes undergo an initial eye exam within five years of diagnosis, while those with type 2 diabetes should have an eye exam at the time of diagnosis. Subsequent exams should be performed annually or more frequently, depending on the severity of the condition.
Screening Methods and Treatment Options
Screening for diabetic retinopathy typically involves a comprehensive eye exam, including visual acuity testing, dilated fundus examination, and optical coherence tomography (OCT). Dilated fundus examination allows the ophthalmologist to visualize the retina and identify any abnormalities. OCT provides detailed cross-sectional images of the retina, helping to detect subtle changes in the retinal structure.
Treatment options for diabetic retinopathy vary depending on the stage of the condition. In the early stages, controlling blood sugar levels, blood pressure, and cholesterol can help slow the progression of the disease. As the condition advances, treatment may involve laser photocoagulation to seal leaking blood vessels, intravitreal injections of medications to reduce swelling and prevent the growth of new blood vessels, or vitrectomy surgery to remove blood and scar tissue from the vitreous gel inside the eye.
Yale Medicine experts stress that proactive management of diabetes and regular eye exams are essential for preserving vision and preventing blindness from diabetic retinopathy. Individuals with diabetes should work closely with their healthcare providers to optimize their blood sugar control and adhere to recommended screening schedules.
Image Source: Google | Image Credit: Respective Owner