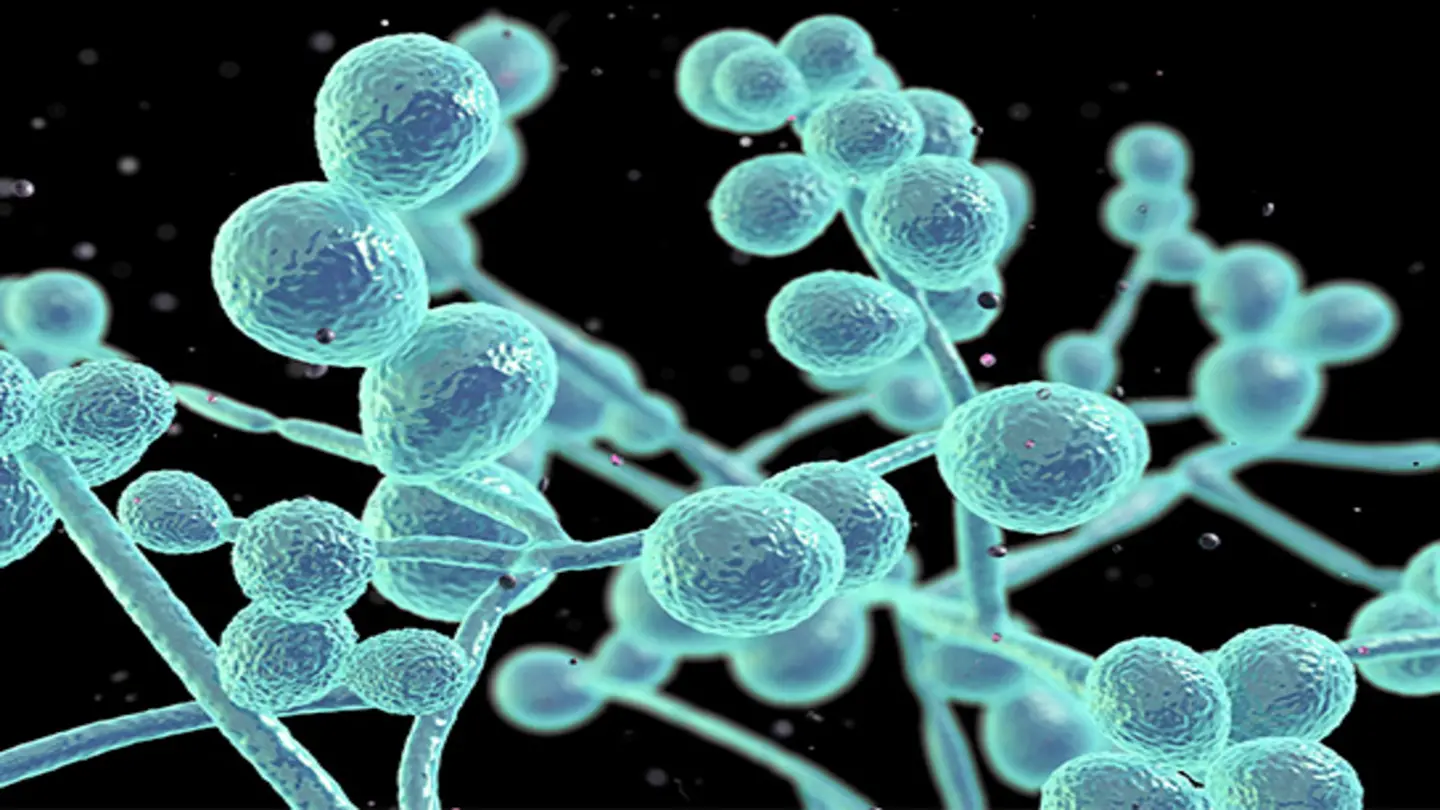
A concerning rise in cases of Candida auris, a multi-drug resistant fungus dubbed the “zombie fungus” due to its resilience, is prompting global health alerts. The fungus, first identified in 2009, is spreading at an accelerating rate, with recent data indicating a significant increase in infections across multiple continents.
C. auris is particularly dangerous because it is often resistant to common antifungal medications, making treatment challenging and increasing the risk of mortality. It can cause severe infections, including bloodstream infections, wound infections, and ear infections, particularly in individuals with weakened immune systems, such as those in hospitals or long-term care facilities.
The Centers for Disease Control and Prevention (CDC) has been tracking the spread of C. auris and has reported a notable uptick in cases in the United States. The fungus is not considered highly contagious person-to-person, but it can spread through contact with contaminated surfaces or healthcare equipment. This makes strict infection control measures crucial in preventing its dissemination.
What sets C. auris apart is its ability to survive on surfaces for extended periods, even after routine cleaning. This persistence contributes to its ability to spread within healthcare settings. The fungus also exhibits a remarkable capacity for genetic mutation, leading to the development of new strains with varying levels of drug resistance.
Global Spread and Concerns
The fungus has been identified in over 30 countries, including India, Pakistan, South Africa, Russia, and several European nations. The initial outbreaks were linked to healthcare facilities, but there is growing evidence of community spread in some regions. This broader dissemination raises concerns about the potential for more widespread infections and the strain on healthcare systems.
Experts are particularly worried about the fungus’s ability to “eat” through the human body, as the nickname suggests, though this is a metaphorical description of its invasive nature. It doesn’t literally consume tissue, but it aggressively colonizes and damages cells, leading to severe illness. The infection often presents with non-specific symptoms, making early diagnosis difficult.
The CDC recommends thorough cleaning and disinfection of healthcare facilities, rapid identification of infected patients, and implementation of stringent infection control protocols. These measures include isolating infected individuals, using personal protective equipment, and screening high-risk patients.
The increasing prevalence of C. auris underscores the urgent need for new antifungal drugs and improved diagnostic tools. Research is underway to develop more effective treatments and to understand the mechanisms behind the fungus’s drug resistance. Public health officials are also emphasizing the importance of antimicrobial stewardship to prevent the overuse of antifungal medications, which can contribute to the development of resistance.
The situation demands a coordinated global response to contain the spread of this potentially deadly fungus and protect vulnerable populations. Continued surveillance, research, and implementation of effective infection control measures are essential to mitigate the threat posed by Candida auris.
Image Source: Google | Image Credit: Respective Owner