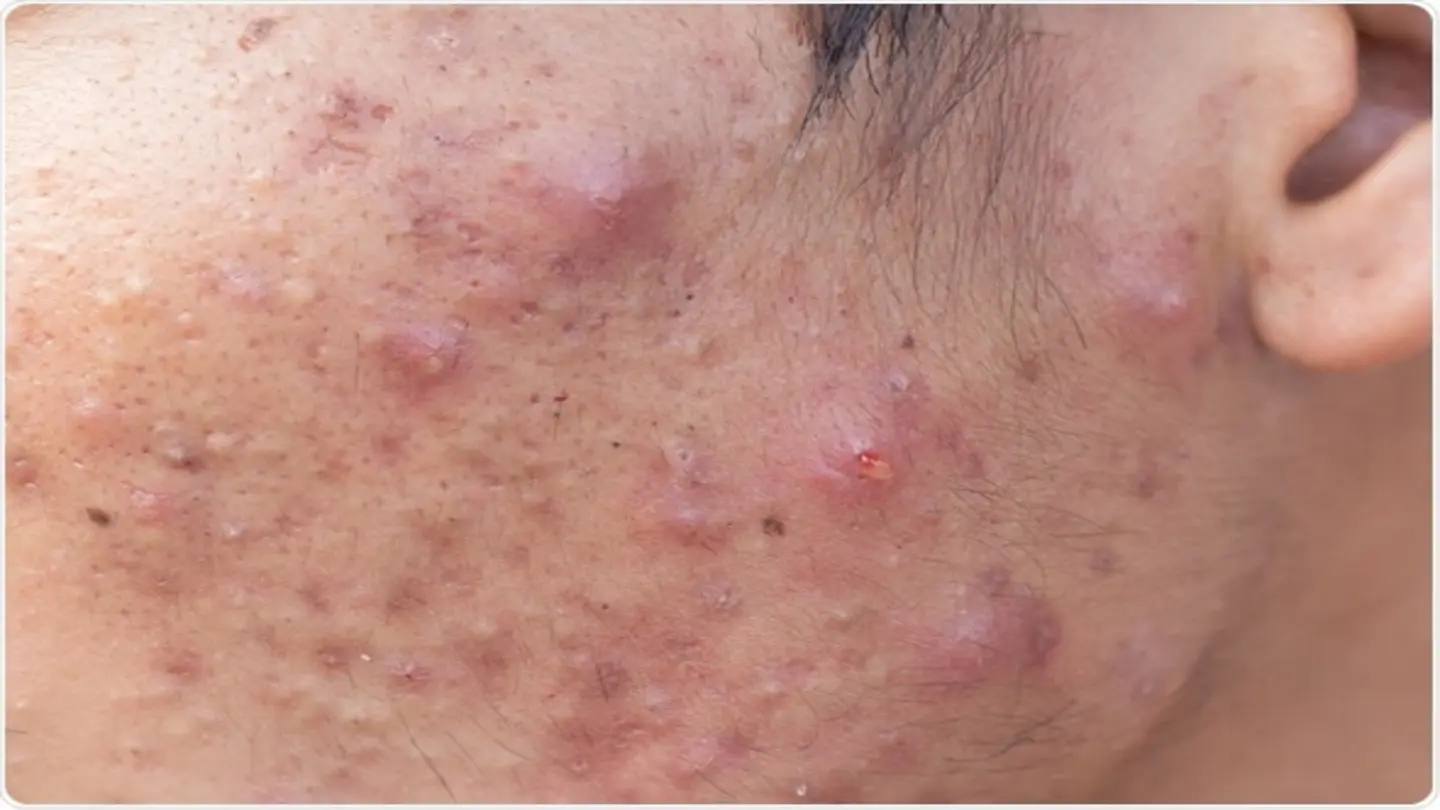
Acne, a common skin condition, often dismissed as a mere cosmetic issue, can sometimes be an indicator of underlying health problems. Beyond the typical teenage breakouts, persistent or unusual acne patterns may signal hormonal imbalances, digestive issues, or other systemic conditions that warrant medical attention. Recognizing these potential connections can lead to earlier diagnosis and more effective treatment.
Digestive Issues
The gut-skin axis highlights the close relationship between the digestive system and skin health. Inflammation or imbalances in the gut microbiome can manifest as acne. Conditions like leaky gut syndrome or inflammatory bowel disease (IBD) can trigger systemic inflammation, leading to skin eruptions. Acne located around the mouth and jawline may be particularly indicative of digestive issues. Probiotic supplements and dietary changes, such as reducing processed foods and increasing fiber intake, can improve both gut health and skin clarity. Consulting a gastroenterologist is advisable for persistent digestive symptoms.
Hormonal Imbalances
Hormonal fluctuations, particularly those involving androgens like testosterone, are notorious for triggering acne. Polycystic ovary syndrome (PCOS), a common endocrine disorder affecting women, is often associated with acne, along with irregular periods, hirsutism (excessive hair growth), and weight gain. In men, hormonal imbalances can also contribute to acne, particularly during puberty and periods of stress. Blood tests to assess hormone levels, along with appropriate medical intervention such as hormonal birth control pills for women or anti-androgen medications, can help manage hormonally driven acne. An endocrinologist can provide specialized care for hormonal disorders.
Inflammatory Conditions
Chronic inflammation in the body can manifest in various ways, including acne. Conditions like rheumatoid arthritis or lupus, characterized by systemic inflammation, can exacerbate skin problems. Inflammatory cytokines, released during these conditions, can stimulate sebum production and clog pores, leading to acne breakouts. Identifying and managing the underlying inflammatory condition is crucial for improving skin health. Medications like nonsteroidal anti-inflammatory drugs (NSAIDs) or corticosteroids may be prescribed to reduce inflammation. A dermatologist and rheumatologist can work together to manage both the systemic condition and its cutaneous manifestations.
Stress and Mental Health
Stress is a well-known trigger for acne. When the body experiences stress, it releases cortisol, a hormone that can increase sebum production and inflammation. Chronic stress can disrupt the skin’s natural barrier function, making it more susceptible to acne-causing bacteria. Managing stress through techniques like meditation, yoga, or therapy can significantly improve skin health. Additionally, addressing underlying mental health conditions such as anxiety or depression is important, as these can contribute to chronic stress and inflammation. Cognitive behavioral therapy (CBT) and mindfulness-based interventions can be effective in reducing stress and improving overall well-being. A holistic approach that addresses both physical and mental health is essential for managing stress-related acne.
Image Source: Google | Image Credit: Respective Owner